
Hoag Memorial Hospital Presbyterian
1 Hoag Drive, Building #41
Newport Beach, CA 92663
949-722-6237
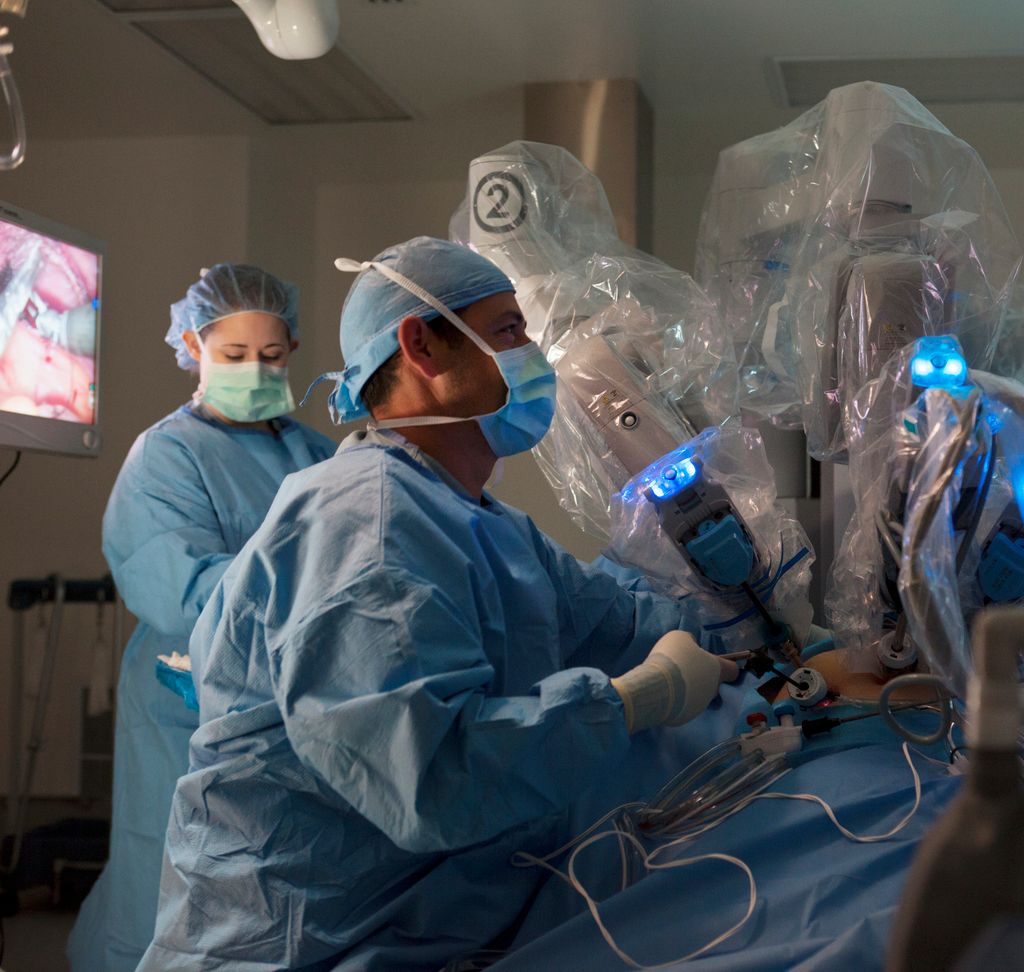
Hoag’s robotic program offers state-of-the-art technology and expertly trained, board-certified lung cancer surgeons.
Hoag offers early-phase clinical trials, including options for lung cancer, that provide access to innovative therapies beyond standard care, guided by specialized oncologists and a dedicated research team.
Hoag’s integrated care network will support you every step of the way through an individualized treatment plan, designed by experts who specialize in your specific type and stage of cancer.



1 Hoag Drive, Building #41
Newport Beach, CA 92663
949-722-6237

16105 Sand Canyon Ave.
Irvine, CA 92618
(949) 722-6237

1 Hoag Drive, Building #47
Newport Beach, CA 92663
949-764-1880

19582 Beach Blvd., #219
Huntington Beach, CA 92648
714-477-8130
Get care from medical providers that fit your needs in a location near you.
Find a providerFind information made to guide and support you on your journey.
See all resourcesDidn’t see what you’re looking for? Reach out and we’ll make sure you get what you need.
Contact usHoag’s Lung Cancer Screening Program is recommended for both current and former smokers, following the recommendations listed above. Read more about Hoag’s Lung Cancer Screening Program.
Hoag’s Lung Cancer Screening Program is through physician referral only. Medicare and other insurance carriers will reimburse the cost of lung cancer screening for patients who meet certain criteria. This criteria includes: being between the ages of 50-77, having smoked at least the equivalent of one pack of cigarettes per day for 20 years. Medicare also requires that you and your physician discuss low-dose CT scan screening, and if it is right for you. Feel free to read through our Shared Decision-Making brochure, to help lead the conversation.
Hoag also offers a service focused on the discussion and assessment if lung cancer screening is right for you. This appointment with a nurse navigator reviews medical history, lung health history, among other things, to complete this Shared Decision Making step. Your physician may refer you to this service, or you can refer yourself. To schedule a Shared Decision Making appointment through Hoag’s Lung Screening Program, please call (949) 7-CANCER.
To learn more about Hoag Lung Cancer Screening Program, please call Lung Cancer Nurse Navigator Mandy Gutierrez, CSN, RN, OCN at (949) 764-7119.
Hoag Family Cancer Institute aligns with national medical societies and government organizations, recommending annual, low dose chest CT screening in patients 50-77 years old with a history of heavy smoking (greater than 20 pack-years*) who currently smoke or have quit within the past 15 years.
Annual screening is currently recommended for this population by the National Comprehensive Cancer Network, along with the American Academy of Family Physicians and the U.S. Preventive Services Task Force.
The above recommendations should take into account issues such as co-existing illnesses and life expectancy, and should be discussed with your physician. Screening should be discontinued if a person develops a health problem that substantially limits life expectancy or the ability or willingness to have curative lung surgery. Hoag encourages you to use this Shared Decision-Making brochure in your conversation.
*Pack year refers to number of packs smoked per day, multiplied by number of years smoked.
Hoag Family Cancer Institute is committed to the prevention and early detection of lung cancer. One of the best ways to prevent lung cancer is to never start smoking, or if you are smoking – stop. Hoag offers an extensive smoking cessation program and many resources to help individuals to stop smoking. Learn more about Hoag’s Smoking Cessation Program.
Designed to meet the educational and emotional needs of lung cancer patients and their families. The support group meets virtually once per month. View virtual meeting dates here.
Since early lung cancers usually do not exhibit symptoms, by the time symptoms occur, the cancer has often spread (metastasized). The treatment success for metastatic lung cancer can be limited. However, patients with stage 1 lung cancers, or early small lung cancers, detected before spreading, have much better survival rates.
A chest X-ray is an X-ray picture taken of the chest, one image from the back and one from the side. The X-rays form an image of the chest including the lungs, but other structures like the heart and spine, may obscure parts of the lungs where a cancer might be. Chest X-rays have not been shown to be useful for the early detection of lung cancer.
CT imaging utilizes a doughnut-shaped camera (scanner). The CT scanner takes several cross sectional images of the chest. CT imaging results in a more complete picture, it’s as if your body is loaf of bread, and we’re taking one slice of bread at a time and looking at the face of it, and then we continue looking at the face of each slice through the whole loaf.
When screening healthy smokers or former smokers for lung cancer, only the lungs need to be viewed. As a result, the radiation administered during the scan can be lowered to about one-sixth of what is given during a conventional CT scan.
No. The best way to prevent lung cancer is to not smoke, and if you are currently smoking, the best thing to do is quit.
A smoker who stops smoking will significantly reduce his/her risk of lung cancer. However, the risk of cancer will not decrease to the low risk of someone who has never smoked.
First, a physician referral is required. During the imaging test, you will need to lie down on the CT table and hold your breath for about 10 – 15 seconds, while the images are taken. Your results will be provided to your referring physician, who will review them with you during a follow-up consultation.
Many individuals will have a nodule from an old infection, or a scar, which can be difficult to distinguish from a very early cancer. In these cases, the patient will be referred to a pulmonologist for consultation and will need to come back for a follow-up scan in 6 -12 months (based on physician recommendation) to make sure the nodule isn’t growing.
Chemotherapy/Systemic Therapy
Chemotherapy uses powerful drugs or chemicals to directly attack cancerous cells. Systemic Therapy is a non-surgical treatment option for cancer patients. Systemic therapy is when drugs are administered into a patient’s blood stream to stop or slow the growth of cancerous cells. Biological therapy, also referred to as “Immunotherapy” utilizes the body immune system to fight cancer cells.
Interventional Pulmonology
Interventional Pulmonology is a different approach to treating and managing lung cancer and other conditions of the respiratory system. While still a relatively new field, Interventional Pulmonology is dedicated to less-invasive methods of diagnosing, treating and managing lung cancer and its symptoms.
Stereotactic Body Radiation Therapy (SBRT)
Stereotactic Radiation Therapy (SRT) is an intermediate technique, with many of the characteristics of both Stereotactic Radiosurgery (SRS) and Image-Guided Intensity-Modulated Radiation Therapy (IG-IMRT). When applied outside of the brain, this technique is often called Stereotactic Body Radiation Therapy (SBRT).
Radiation Oncology
Hoag’s Radiation Oncology Program offers the widest range of radiation therapy options available, ensuring every treatment plan is precisely tailored to each patient.
Precision Medicine Program
Hoag’s Precision Medicine Program combines genomics and genetics to diagnose, treat, and prevent diseases. Using the latest advances in genomic technologies, targeted therapies and research, our precision medicine program brings together a multidisciplinary team, including a robust genetic counseling group of experts, to provide patients with the latest in innovation and technology.
Tumor Boards
Tumor boards* are a meeting of Hoag’s top experts in their respective subspecialties to determine the best approach for a patient’s individual cancer case.
Palliative Care
Palliative care is a specialty that focuses on improving the quality of life of individuals facing serious illness through medical management and emotional support.
Cancer Clinical Trials
Early development clinical trials (phase I and II) are novel drug therapies that examine new treatments that provide options beyond standard of care. During these trials, researchers are carefully examining the best way to administer the treatment, determine how much can be safely given, identify important potential side effects, as well as assess cancer response.
As the area’s highest-volume cancer center, Hoag Family Cancer Institute sees, diagnoses and treats more lung cancer patients than any other hospital in Orange County—including patients with rare subtypes and complex cases. That gives Hoag a deep well of experience, which can lead to more accurate staging, more personalized treatment plans, fuller recoveries and better outcomes. Hoag’s commitment to research and the latest treatment options have improved survival rates for patients treated at Hoag at every stage of lung cancer.
If you are concerned about lung cancer due to a long history of heavy smoking, Hoag’s Early Lung Cancer Screening Program might be right for you. This groundbreaking program catches lung cancer in high-risk patients earlier through annual, low-dose CT screenings for heavy smokers or former heavy smokers between 50-77 years of age. Some private insurance plans and Medicare pay for this vital preventative screening.
After discussing your symptoms and medical history with your doctor, you will likely be given a thorough medical exam, which may be followed by other tests and diagnostic procedures. At Hoag, this may include:
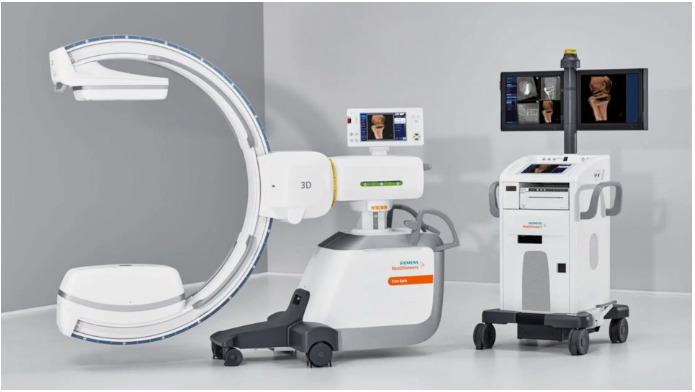
Cios Spin, a new imaging technology for diagnosing lung cancer earlier, more accurately and less invasively. Hoag is the first hospital in Orange County to offer this technology.
The Ion Robotic-Assisted Bronchoscopy Platform, a robot-enabled technique allowing for safe, minimally invasive collection of tissue samples for biopsy. Hoag is one of the few Interventional Pulmonology programs in the U.S. offering this technology.
Endobronchial Ultrasound (EBUS), a minimally invasive procedure used to obtain lymph node tissue samples for biopsy without conventional surgery.
Convex-Probe Endobronchial Ultrasound Bronchoscopy (CP-EBUS)
Radial-Probe Endobronchial Ultrasound Bronchoscopy (RP-EBUS)
Ion Navigational Bronchoscopy, a recent innovation that extends the conventional bronchoscope, providing doctors with better views of cancerous lesions deep in the lungs.
Cone-Beam Computed Tomography (CBCT) with 3D Fluoroscopy
Positron Emission Tomography (PET)
Bone Scans
Mediastinoscopy
After diagnosis, your doctor will talk to you about your current symptoms, discuss treatment options and potentially refer you to a specialist for more tests or surgery. If you still smoke or use tobacco at the time of your diagnosis, quit immediately.
Treatment options for lung cancer depend on many factors, including how advanced the cancer is when detected, your age and any other health issues you may have. The treatments Hoag recommends for lung cancer vary from patient to patient, but may include:
Cell Therapy (Immunotherapy)
Systemic Therapies (chemotherapy & biotherapy)
Active Surveillance
Hoag is committed to leading the way in state-of-the-art technologies and advanced treatment options. Part of this commitment includes clinical research with the goal of helping patients live longer, healthier lives. Through carefully planned clinical trials, researchers evaluate the safety and effectiveness of new ways to diagnose, treat and prevent diseases or conditions. Treatments studied in clinical trials might be new drugs or new combinations of drugs, new surgical procedures or devices, or new ways to use existing treatments.

Director, Hoag Lung Cancer Program, Thoracic Surgery

Thoracic Surgery

Medical Oncology

Medical Director, Neuro-Oncology

Co-Director of Early Phase Development Therapy, Director of Lung and Head & Neck Cancers

Co-Director, Breast Medical Oncology

Interventional Pulmonology

Medical Director, Radiation Oncology Program

Radiation Oncology

Radiation Oncology

Radiation Oncology

Radiation Oncology

James & Pamela Muzzy Endowed Chair in Molecular Imaging and Therapy

Diagnostic Radiology, Nuclear Medicine

Clinical Nurse Navigator
Hoag’s Precision Medicine Program combines genomics and genetics to diagnose, treat, and prevent diseases. Using the latest advances in genomic technologies, targeted therapies and research, our precision medicine program brings together a multidisciplinary team, including a robust genetic counseling group of experts, to provide patients with the latest in innovation and technology.
Hoag’s Molecular Imaging & Therapy (MIT) Program has been recognized as one of only 95 Radiopharmaceutical Therapy Centers of Excellence in the world. Through this program, Hoag is helping pioneer the most sensitive imaging methods to date to advance research and applications of molecular imaging and therapy in the treatment of cancer patients. These trials are expected to play a significant role in cancer detection, individualized treatment and drug development. The future of cancer detection and therapy is offered today at Hoag.
Hoag Family Cancer Institute provides a dedicated team of genetic counselors that offer hereditary cancer assessment, offering risk assessment and genetic cancer testing to those with a personal or family history of cancer.
Being diagnosed with cancer can feel overwhelming at times. Many patients and their families need help with coping and can benefit from supportive counseling. Oncology Clinical Social Workers are available to provide emotional and practical support during all stages of cancer including diagnosis, treatment and post-treatment survivorship.
Hoag Family Cancer Institute dietitians work closely with patients’ physicians, nurses, therapists, and social workers to ensure complete care.
Hoag is the top choice for cancer care in Orange County, with cancer survival rates that continually exceed national averages. Our dedicated, world-class teams are wholly focused on helping you survive cancer, heal and move forward with your life.
Lung cancer is cancer that begins in the lungs, the main respiratory organs of the body. It can sometimes spread to other organs and lymph nodes. Today, lung cancer is the third most common cancer in the United States, according to the CDC.
The are two main types of lung cancer:
Small cell lung cancer (SCLC), includes two types that include many different types of cells. This type accounts for 15 percent of lung cancer cases. The cancer cells of each type grow and spread in different ways. The types of small cell lung cancer are named for the kinds of cells found in the cancer and how the cells look when viewed under a microscope:
Small Cell carcinoma (oat cell cancer)
Combined small cell carcinoma
Non-small cell lung cancer (NSCLC), which is the most common type of lung cancer, accounting for about 85 percent of lung cancer cases. Subtypes of NSCLC include adenocarcinoma, squamous cell carcinoma and large cell carcinoma
Several common cancers that begin elsewhere in the body can spread (or metastasize) to the lungs, including skin, breast, kidney and pancreas cancers.
The symptoms of lung cancer can be different for every patient, and vary based on how advanced the cancer is. Common symptoms can include:
Recurring bronchitis, pneumonia and other respiratory infections
Swollen lymph nodes in the chest
Chest pain
A constant or recurring cough
A raspy or hoarse speaking voice
Wheezing
Unexplained shortness of breath
In more advanced lung cancer cases, symptoms may include:
Unexplained fatigue, loss of appetite and weight loss
Coughing up blood, or mucus that’s reddish brown
Recurring headaches that can be severe
Moderate to severe aches in the bones and chest
Pleural effusion, a condition in which fluid accumulates in the chest cavity around the cancerous lung
There are several risk factors that are believed to increase your risk of developing lung cancers. These include:
Smoking and exposure to secondhand smoke, with most cases of lung cancer being due to tobacco use.
Exposure to radon, a colorless, odorless, naturally-occurring radioactive gas that can seep into and accumulate in homes and workplaces over time
Exposure to asbestos, a naturally occurring mineral that was once used extensively in residential and commercial insulation and is still found in many older buildings.
Previously having lung cancer
A family history of lung cancer
Previous radiation therapy to the chest
Ways to reduce your risk of developing lung cancer include:
Quit smoking and encourage smokers you might live with to not expose you and others to secondhand smoke. Hoag offers a smoking cessation class to support your efforts to quit smoking.
Avoiding radon, including having your home professionally checked. Almost every state in the U.S. has some level of radon. The top ten states with highest average radon concentrations are Alaska, South Dakota, Pennsylvania, Ohio, Washington, Kentucky, Montana, Idaho, Colorado and Iowa.
Avoiding asbestos, including wearing proper protective gear when working around known asbestos and having older buildings and homes checked for asbestos prior to beginning any demolition or renovation work.
Yes, early lung cancer screening is available at Hoag.
If you are concerned about lung cancer due to a long history of heavy smoking, Hoag’s Early Lung Cancer Screening Program might be right for you. This groundbreaking program catches lung cancer in high-risk patients earlier through annual, low-dose CT screenings for heavy smokers or former heavy smokers between 50-77 years of age. Some private insurance plans and Medicare pay for this vital preventative screening.
By submitting this request, you agree to receive communications from Hoag and accept our Privacy Policy and Terms of Use.