Breast cancer screening 101: Answers to your most pressing questions
Early detection remains one of the most powerful tools for maintaining breast health, but just hearing the words “breast screening” causes some women to immediately think of “breast cancer.” It is important to remember that the two are not interchangeable.
“Breast health is a continuum,” says Dr. January Lopez, medical director of breast imaging at Hoag Breast Center. “Most women who come in for screening are healthy and simply making a proactive choice to monitor their health. Screening is about reassurance and early detection, not about assuming that something is wrong.”
Here, Dr. Lopez clarifies the difference between screening, diagnostics, and treatment options so women can navigate breast care with confidence, not fear.
Screening: Looking for problems before symptoms appear
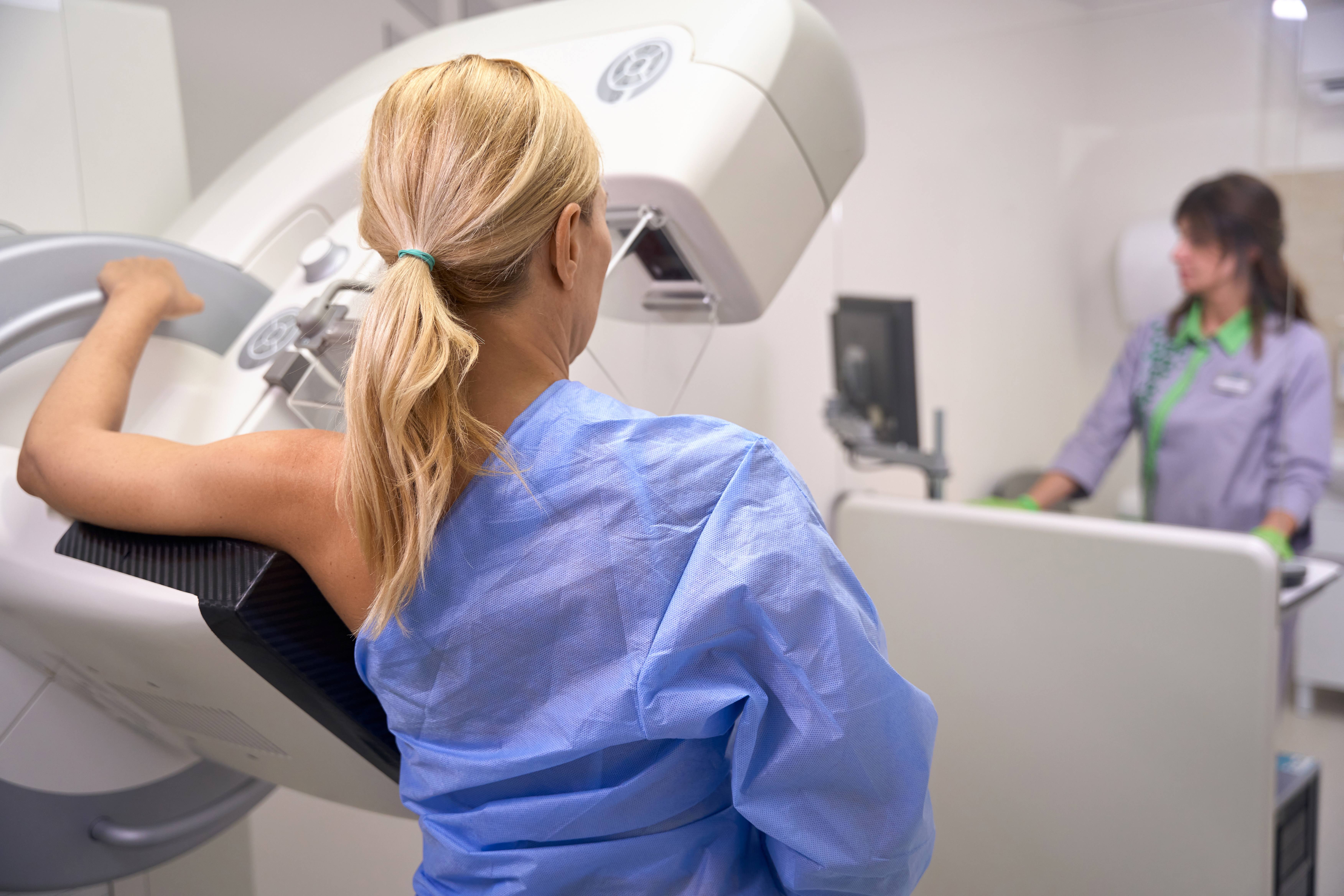
Breast cancer screening is designed to identify abnormalities, which may or may not be early signs of breast cancer. The most common screening tool is a mammogram, which remains the gold standard for early breast cancer detection.
“Mammography allows us to find cancers years before they could be felt during a physical exam,” Dr. Lopez says. “That early detection can dramatically expand treatment options and improve outcomes.”
Experts recommend that most women begin annual screening mammograms by age 40. Even women with no family history should take screening seriously. In fact, most breast cancers occur in women without a family history of the disease.
Diagnostic testing: When something needs a closer look
If a screening exam reveals an area that needs further evaluation, physicians move to diagnostic imaging, which may include targeted mammography, ultrasound, or other advanced imaging tools.
Diagnostic imaging is also used to evaluate areas of clinical concern like a new or enlarging breast lump, nipple discharge, or skin changes that you or your doctor may discover.
“Diagnostic imaging helps us answer a very specific question,” Dr. Lopez says. “Is this finding something harmless, like a cyst or benign change, or is it something that needs further evaluation?”
It’s important for patients to understand that a call-back after a screening mammogram does not mean cancer. In many cases, additional imaging simply provides more detailed views of the breast tissue.
Treatment: Personalized care if cancer is found
If cancer is diagnosed, Hoag’s multidisciplinary team works with each woman to develop a highly individualized treatment plan that may include surgeons, medical oncologists, radiation specialists, and genetics experts.
Advances in breast cancer care have also expanded options for preserving the natural appearance of the breast. Techniques such as oncoplastic surgery combine cancer removal with reconstructive methods to achieve both safe and cosmetically superior outcomes.
Hoag is also at the forefront of clinical trials exploring new therapies and technologies designed to target cancer more precisely and reduce the risk of recurrence.
“The goal is always to tailor treatment to the individual patient,” Dr. Lopez says. “With today’s technology and surgical techniques, many women have more options than ever before.”
Knowledge reduces fear
For many women, anxiety about breast cancer can come from not knowing what to expect.
“When women understand the purpose of each step—screening, diagnostics, and treatment—the process becomes far less intimidating,” Dr. Lopez says. “Our goal is to provide clarity so women can make informed decisions about their health.”